How Should Your GLP-1 Nutrition Change by Age?
Your protein needs at 35 are not the same as at 55. Here's what the evidence says about adjusting your nutrition on Ozempic or Mounjaro as you get older.
Your protein needs at 35 are not the same as at 55. Here's what the evidence says about adjusting your nutrition on Ozempic or Mounjaro as you get older.
Your body processes protein less efficiently as you age, loses muscle faster, and responds differently to caloric deficits — all of which change the nutrition equation on GLP-1 medications. Most GLP-1 nutrition advice treats every user the same. But a 35-year-old starting Ozempic has fundamentally different metabolic needs than a 60-year-old on the same medication.
After 30, you lose approximately 3-8% of muscle mass per decade — a process called sarcopenia. By 50, this accelerates. GLP-1 medications compound the problem: up to 40% of weight lost on semaglutide can come from lean mass. The older you are, the harder it is to rebuild that muscle, and the more dangerous the loss becomes.
There's also anabolic resistance — your muscles become less responsive to the protein you eat. A 25-year-old can trigger muscle protein synthesis with 20g of protein per meal. By 60, you may need 35-40g to get the same response. This means the standard "eat more protein" advice needs to be more specific as you age.
In your 30s and 40s, your primary focus on GLP-1 should be building the habits that will protect you later — particularly hitting 0.7-0.8g of protein per pound of body weight and establishing a consistent strength training routine. You have a metabolic advantage at this age: muscle protein synthesis is still relatively efficient, recovery is faster, and hormonal support for muscle maintenance is stronger.
That doesn't mean you can be careless. GLP-1 appetite suppression still puts your muscle at risk if you're not eating enough protein. The difference is that the margin for error is wider in your 30s than it will be in your 50s.
For a 180-pound person, that's 126-144g daily. Spread across three meals, that's roughly 40-48g per meal. This is enough to maintain muscle mass during GLP-1 weight loss at this age.
Compound movements — squats, deadlifts, rows, presses. At this age, your recovery capacity supports moderate to high intensity. Building muscle now is an investment that pays off significantly after 50.
Use this window to learn what balanced meals look like. Track your protein for a few weeks until you can estimate by sight. People who build these skills in their 30s-40s have much better outcomes long-term.
After 50, you need more protein per meal, more deliberate meal timing, and non-negotiable strength training to counter the accelerating muscle loss that GLP-1 can amplify. This is where nutrition on GLP-1 gets serious. The combination of age-related sarcopenia and medication-induced lean mass loss creates a compounding risk that most people don't anticipate.
Research shows that adults over 50 need 0.8-1.0g of protein per pound of body weight to maintain muscle mass during weight loss — significantly higher than younger adults. On GLP-1, where appetite is suppressed and eating feels like a chore, hitting these targets requires intentional planning.
Hormonal shifts add another layer. Women going through menopause experience declining estrogen, which accelerates both muscle and bone loss. Men see gradual testosterone decline. Both changes mean your body is less able to hold onto muscle during a caloric deficit — exactly what GLP-1 creates. See our menopause + GLP-1 guide for specific strategies.
For a 160-pound person, that's 128-160g daily. At 3 meals, each needs 43-53g of protein. This is genuinely hard with a suppressed appetite — protein shakes, Greek yogurt, and cottage cheese become essential tools.
Rapid weight loss on GLP-1 can reduce bone density. After 50, you need 1,200mg calcium and 1,000-2,000 IU vitamin D daily. Don't rely on supplements alone — dairy, leafy greens, and fatty fish count too.
Due to anabolic resistance, your body can't efficiently use a single 80g protein meal. Three meals with 40-50g each triggers muscle protein synthesis three times per day instead of once. More on protein targets →
The most common mistake is celebrating rapid weight loss without realizing how much of it is muscle. Scale weight drops feel great, but if a significant portion is lean mass — which it often is after 50 — you're trading short-term progress for long-term metabolic damage, frailty risk, and almost certain weight regain.
GLP-1 can suppress appetite so effectively that people over 50 end up eating 800-1,000 calories daily. At this level, muscle loss accelerates regardless of protein percentage. Minimum 1,200-1,400 calories is critical. More on muscle loss risk →
Walking is great but doesn't send the signal to preserve muscle. Resistance training is the only exercise modality that directly counters both sarcopenia and GLP-1 lean mass loss. Even 2 sessions per week makes a measurable difference. Strength training guide →
When you're eating less food overall, every calorie needs to count. Calcium, vitamin D, B12, iron, and magnesium gaps are common in older GLP-1 users. A simple blood panel every 6 months can catch deficiencies early.
If you're losing more than 1-1.5% of body weight per week, the rate may be too aggressive — especially after 50. Talk to your doctor about titrating the dose to balance effective weight loss with muscle preservation.
Protein needs on GLP-1 increase with every decade — from 0.7g/lb in your 30s to potentially 1.0g/lb in your 60s+ — because your muscles become less efficient at using the protein you eat. Here's the breakdown by decade, based on current research on sarcopenia, anabolic resistance, and GLP-1 outcomes.
Muscle protein synthesis is still efficient. Focus on consistency — hitting 25-40g per meal across 3 meals. Recovery from training is quick. Build the foundation.
Anabolic resistance begins. You may notice slower recovery from workouts. Aim for 30-40g per meal minimum. This is the decade to lock in protein-first meal planning if you haven't already.
Sarcopenia accelerates. Hormonal shifts (menopause, testosterone decline) compound the challenge. Each meal needs 35-45g of protein. Leucine-rich sources (whey, eggs, chicken) become especially important for triggering muscle synthesis.
Maximum protein effort. At this age, every gram counts. Supplementing with whey or casein protein between meals can help bridge the gap when appetite is low. Resistance training is absolutely essential — without it, even optimal protein intake won't fully prevent muscle loss.
Protein targets go up, not down, as you get older. And on GLP-1, where eating less is the default, this means being more intentional about every meal — not less. Tracking protein intake, even briefly, is one of the highest-impact habits at any age.
These are real meals from FitMate members on GLP-1 — each one hits the protein targets we're talking about, regardless of age. The key is building every meal around a protein source first, then adding fiber and complex carbs around it.


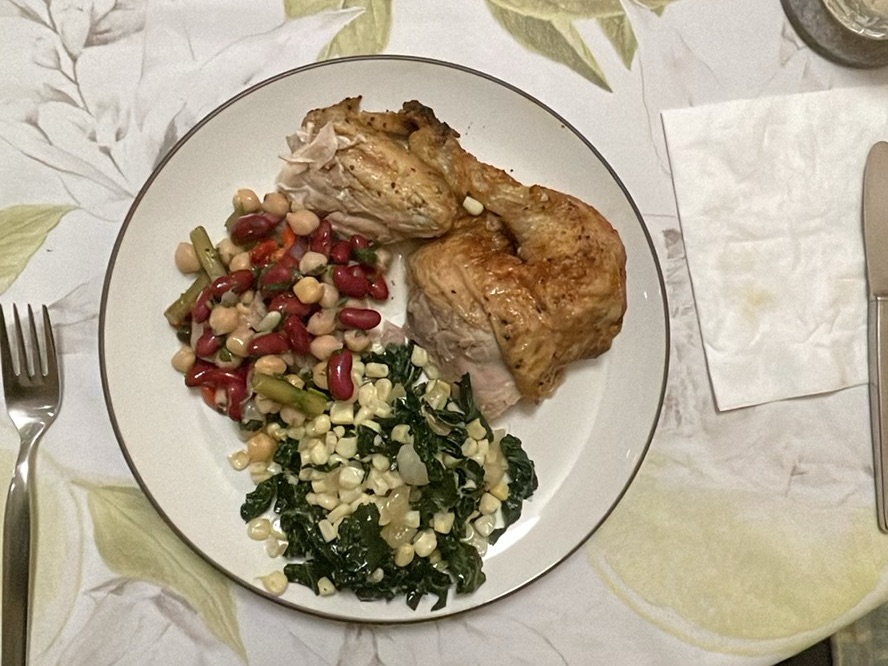
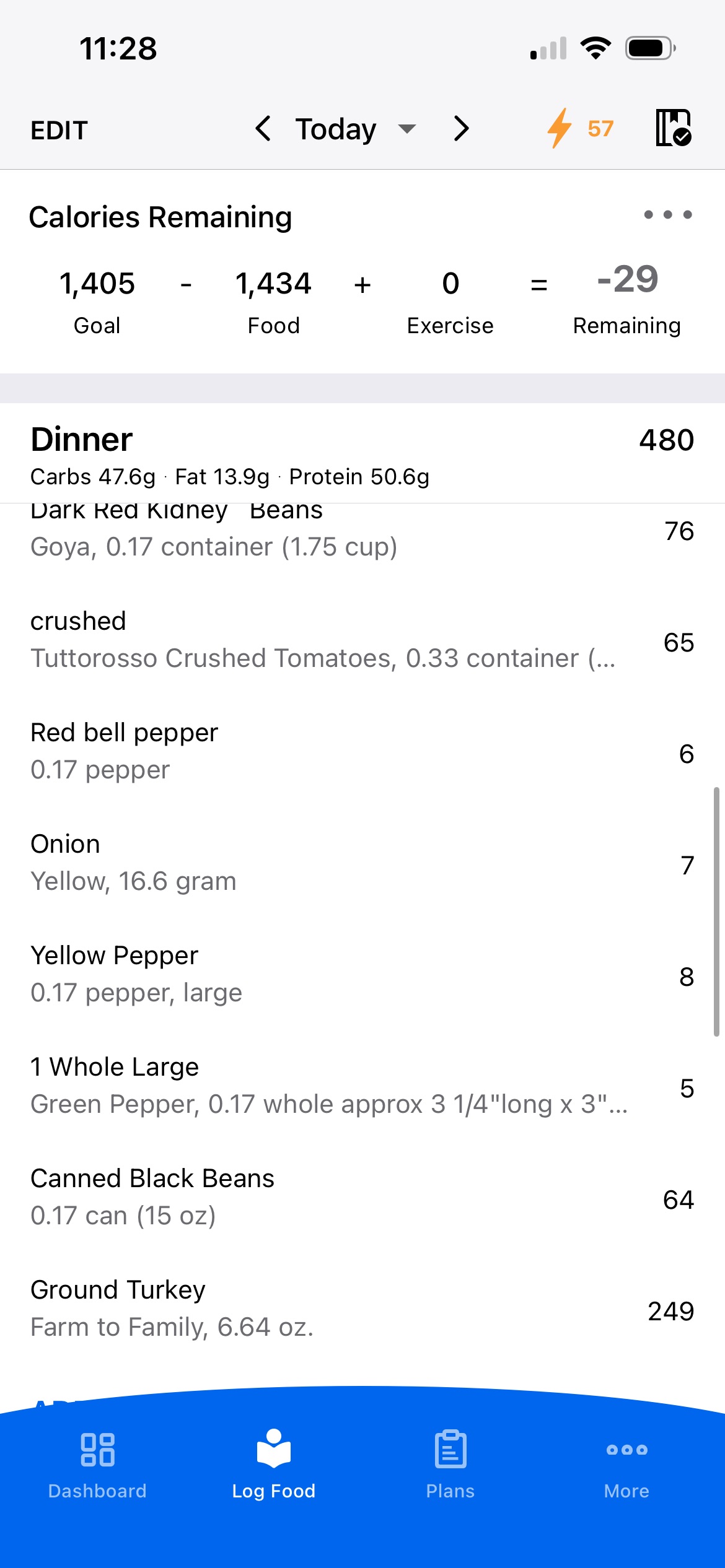
Every meal has 36-44g of protein — enough to hit the per-meal threshold even for people over 50. And they're all under 500 calories. When appetite is suppressed, this kind of nutrient density is exactly what you need.
FitMate Coach builds personalized nutrition plans — AI-powered meal tracking, protein monitoring, and 1-on-1 coaching that understands your specific needs.
Get Started →Get the latest research on weight loss, GLP-1, and sustainable eating habits — no fluff.